The Paleo Diet: Is There Scientific Evidence?

There has been a lot of scrutiny placed on DNA diets, but what about the popular Paleo diet? Has this style of eating been studied in clinical settings? In this post we are going to analyze 3 of the biggest studies that are often cited in support of a Paleo diet. All three of these studies were short term and used a version of the Paleo diet to treat type 2 diabetes and to improve markers of heart health in healthy, middle aged Australians.
One thing that popped out to us as we broke down the studies is that they were relatively low in saturated fats. This is significant because many Paleo influencers tend to advocate for higher amounts of dietary fat than most nutrition guidelines. The diet protocols also reduced total calories and food intake, so it could be that any benefits seen were due to moderate fasting rather than the Paleo diet.
Is there evidence to support the Paleo diet?
The first study on our list used Paleo diet principles to tackle type 2 diabetes.
Paleo Diet Impact on Type 2 Diabetes Study
Study details
- A randomized control trial of 32 patients with type 2 diabetes (“T2D”) from Sweden, also 9 additional individuals for observation
- Average age of 59
- BMI of 25-40
- Followed a Paleo diet for 12 weeks, split in two with one group receiving additional exercise
- Diet as follows: “The diet was based on consuming lean meat, fish, seafood, eggs, vegetables, fruits, berries, and nuts. Cereals, dairy products, legumes, refined fats, refined sugars, and salt were excluded with the exception of canned fish and cold cuts like ham. The diet was consumed ad libitum, with restrictions of the following: eggs (1–2/day but a maximum of 5/week), potatoes (1 medium sized/day), dried fruit (130 g/day), and nuts (60 g/day). Rapeseed or olive oil (maximum 15 g/day) and small amounts of honey and vinegar were allowed as flavoring in cooking. Participants were instructed to drink mainly still water. Coffee and tea were restricted to a maximum of 300 g/day, and red wine to a maximum of one glass/week.”
The results
There is only a single figure in this paper relating to the results so it’s straightforward to get on with the analysis. The graph below shows measures for fat mass, HOMA-IR (a way of measuring β-cell function and insulin resistance, so an output for T2D severity), for these lower is better. The authors also measured VO2 max (the maximum amount of oxygen an individual can use during strenuous exercise, so a measure of fitness) and maximal workload (again a measure of fitness), for these two higher is better. 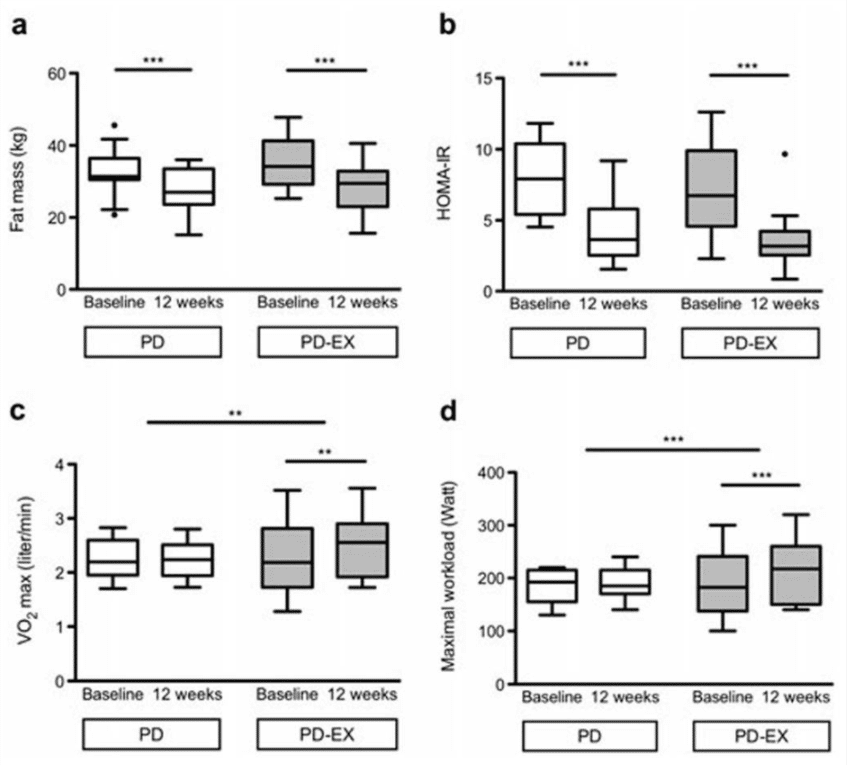
What do the authors say?
Based on our results, we conclude that the Paleolithic diet is a powerful tool to improve fat mass and metabolic balance including insulin sensitivity, glycemic control, and leptin in individuals with type 2 diabetes. Supervised exercise training did not provide additional effects on these outcomes, but preserved lean mass in men and increased cardiovascular fitness. Detailed analyses of tissue-specific effects of these interventions, including putative effects on hepatic versus muscle insulin sensitivity, are of further interest.
Are there any criticisms of the study?
There are a few criticisms that can be leveled at the study (and as a trend you’ll notice the same comments throughout this post). The study message is actually very clear, but the message might be at risk of being oversold in the podcast and blog world.
No healthy control
The study was performed in a population with T2D, and the main effects were based around observations between those following a paleolithic diet with an without extra exercise. The inclusion of an observation only group is to be applauded but healthy baseline controls would be more useful.
Small sample size
There is no getting around the fact that the groups are small. Larger scale studies are desirable, especially in “healthy” populations, but are sadly lacking.
Short duration
Twelve weeks is a relatively short duration, but the effects observed are very interesting. It would be good to see measurements over a longer time course and again in a “healthy” population.
Effect of calorie restriction/Paleolithic specific?
This is a point the authors themselves address. A major change in the Paleo diet of those in the study was a reduction in carbohydrates and saturated fats, and an increase in protein, monounsaturated fatty acid and polyunsaturated fatty acid intake. But interestingly, in this study both groups reported a significant reduction in total energy intake (~410kcal/day reduction), could it be this that is driving the effect rather than the specific aspects of the paleolithic diet? Calorie restriction (to a greater extent than this study) has certainly shown profound benefits. 1
Our take
We’re actually pretty strongly on board with this study, while small in scale and hampered by a lack of healthy controls (to extrapolate to the wider population), the evidence that a Paleo diet (as defined by the study) can be beneficial for those with T2D is certainly strong. However, what is not clear is whether the effect is driven by changes in carbohydrate/fat intake or by the overall total reduction in calories. It is most likely that it’s a combination of factors are proving beneficial with the exact contribution of each remaining unknown. One interesting aside is that in this study the participants saturated fat intake was actually significantly reduced (as was overall fat intake, but not significantly so). Therefore this paper doesn’t fit in with a narrative suggesting that saturated fat intake is beneficial (it also doesn’t present any counter evidence that it’s harmful), or that it doesn’t affect triglycerides, HDL and LDL. Finally, it is important to remember that this study was performed in people with T2D, and so we shouldn’t really extrapolate the findings into health individuals. Moving on lets look at some work performed in a healthy population.
The Paleo Heart Study
Study details
- Randomised control trial of 39 healthy women in Australia
- Mean age of 47 and a mean BMI of 27
- Randomized into either a paleolithic or traditional healthy diet (Australian Guide to Healthy Eating – AGHE) for 4 weeks
- For the paleo arm this entailed: “…lean meats, fish, eggs, nuts, fruits and vegetables, and small amounts of olive or coconut oils. Grains, cereals and dairy products were not permitted. Dairy products were replaced with unsweetened almond milk. Sugarless black coffee and tea were allowed. All vegetables were permitted on the diet, except for corn, white potatoes and legumes. To ensure adequate carbohydrate, additional fruit was recommended. Dried fruit was limited to one tablespoon per day.”
- The traditional healthy diet involved: “…increasing vegetable and fruit intake and whole grain products, reducing fat intake, and consuming low fat dairy products. Advice was also given to reduce intake of discretionary food items such as cakes, biscuits, sugary drinks and candy…”
The results
No figures in this paper, but rather a couple of tables detailing various physical and biochemical measurements. The take home message for physical measurements is that both overall weight and waist circumference decreased in both diets, with a significantly greater decrease in the Paleo diet group (3.2 kg drop in paleo, 1.21kg in AGHE, 3.35 decrease in paleo and 1.55 in AGHE). The authors ascribe this to the increased protein intake associated with the paleo diet. Things were less dramatic for the biochemical markers. Participants in both dietary groups experienced reductions in total cholesterol (0.55 mmol/L drop in paleo, 0.41 in AGHE) and LDL cholesterol (0.40 mmol/L decrease in paleo and 0.26 in AGHE), however, there were no significant differences in these changes between the dietary groups. Interestingly those following the paleo diet saw a reduction in triglycerides (0.18 mmol/L reduction) whereas no significant effect was seen in the AGHE group. There were no significant differences between dietary groups in other biomarkers of metabolism (fasting C-reactive protein, glucose, insulin, urinary sodium or creatinine) and no notable changes in serum α-carotene or lycopene. Some interesting findings came out of the dietary intake study as well. As may be expected, the paleo diet derived significantly more energy from protein (4.67% more) and fat (9.39% more) than the AGHE group, which in turn derived significantly more from carbohydrates (14.63% more in AGHE). There were no significant differences in the various fat groups, although once again the Paleo diet group consumed less saturated fat, and this also accounted for less of the daily energy, but not significantly so in either case (a greater increase in baseline was seen in the AGHE diet, so this may account for the lack of significance). Importantly both diets maintained fiber intake, and both managed just under 25g, the important number if you read this previous post. Finally, looking at micronutrients, as you might expect based on the dietary attributes, those on the paleo diet had significantly less iodine, sodium and calcium, whereas they had significantly more β-carotene.
What do the authors say?
In healthy females, the Paleolithic diet induced a more favorable effect on body composition over the short term intervention period.
Are there any criticisms of the study?
Again, this study has a small sample size and short duration. Perhaps another criticism is that the version of the Paleo diet studied is not the the version of the Paleo diet followed by most people. It’s hard to fairly classify this study as a true Paleo study.
Our take
Again, another interesting, albeit small, study showing some interesting effects. The most striking outcome is that there was no difference in various lipid markers between the diets, an effect which has been seen in previous other studies. One potential explanation is that these other studies involved less healthy individuals, or were smaller scale, however this study is not much larger, and so it becomes difficult to draw a firm conclusion. One take could be that there are other factors which modulate the various lipids in conjunction with dietary changes, and effect which is borne out by the variation reported in this paper. From a saturated fat angle the authors report significant reductions in total and LDL cholesterol for both diet groups, and a reduction in triglycerides for the paleo diet, however they remain concerned about the total fat, and saturated fat intake for both diets, which again were remarkably similar between the diets. To answer this question we’re going to need bigger and longer running studies, which will most likely be epidemiological and retrospective in nature (as with those we have covered previously) due to the issues and costs involved in running large scale randomized control trials for nutrition in healthy individuals.
The Paleo Diabetes Study
Paleolithic nutrition for metabolic syndrome: systematic review and meta-analysis
Study details
- A systematic review of four randomized control trials involving 159 participants with metabolic syndrome (a cluster of 5 risk factors [waist circumference, blood pressure, and serum cholesterol, HDL and glucose] which often occur together and are precursors for T2D.
- Eligible trials had to be based on the following: “Our specific inclusion criteria for a Paleolithic nutritional pattern were that it comprised vegetables (including root vegetables), fruit (including fruit oils, e.g., olive oil, coconut oil, and palm oil), nuts, fish, meat, and eggs, and it excluded dairy, grain-based foods, legumes, extra sugar, and nutritional products of industry (including refined fats and refined carbohydrates).”
- Control diets were based on current national dietary guidelines in the country the study was based in.
The studies used those by Lindberg et al3, Jonsson et al4 and Mellberg et al5, all based in Sweden and finally Boers et al, from the Netherlands6.
The results
A huge figure to start us off and once again we’re looking at some forest plots (forest plots were catapoulted to fame in the infamous Chris Kresser vs. James Wilkes debate on the Joe Rogan podcast last year). The black square for each study represents the mean with the variation shown by the horizontal line, the pooled effect is then shown with the diamond below. To the left of the vertical line favors the paleo diet, and to the right the control diet. 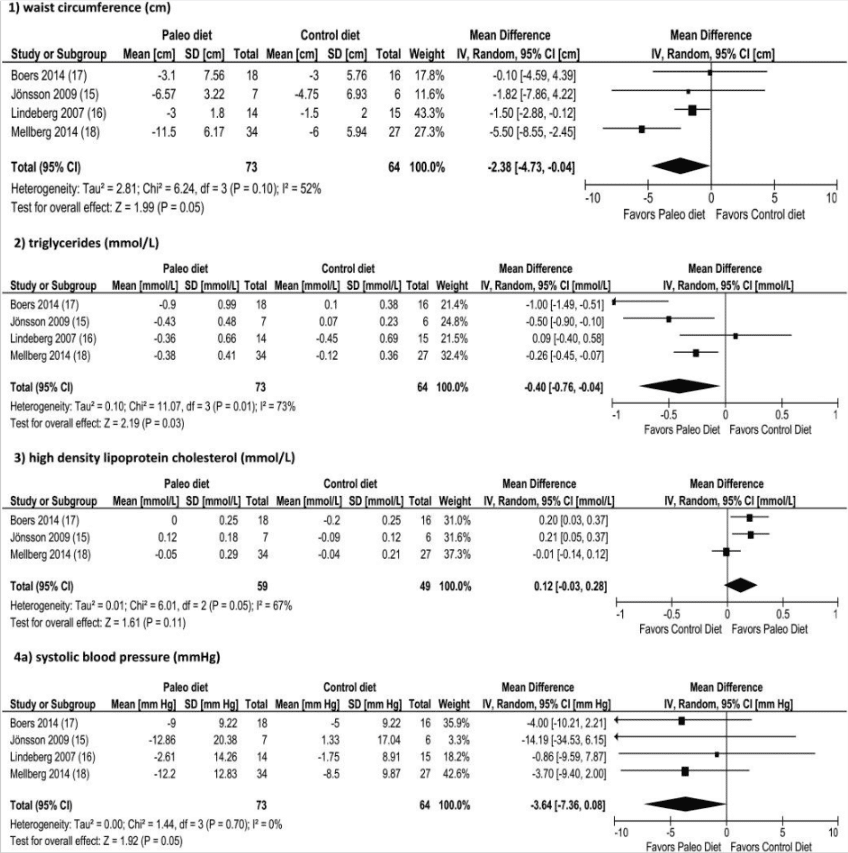
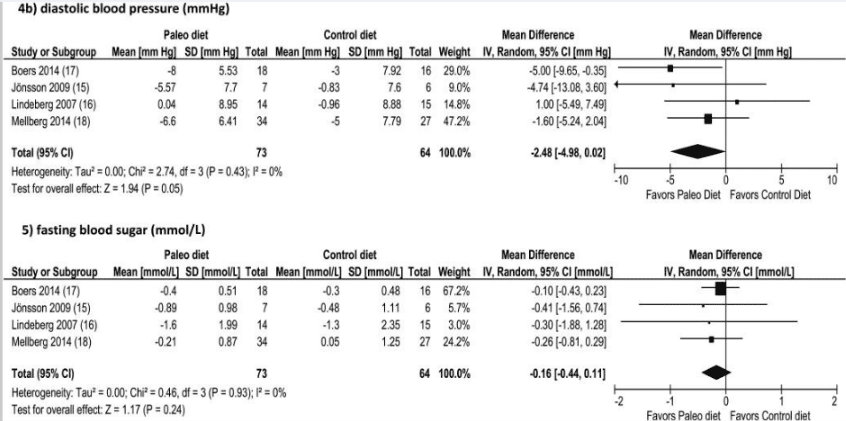
What do the authors say?
In conclusion, state-of-the-art nutritional science readily explains the metabolic benefits of a (modest) restriction of carbohydrates, a lack of high–glycemic index products, a low ω-6 over ω-3 fatty acid balance, and a reduction of salt intake in patients with insulin resistance and the metabolic syndrome. In contrast, it is less clear whether the avoidance of whole grains and dairy products is a prerequisite for the optimal control of metabolism. Although numerous small-scale pathophysiologic studies have highlighted their potential adverse health effects, large-scale epidemiologic data suggest that whole grain- and (fermented) dairy consumption protect against diabetes. Future studies should carefully examine the importance for health of avoiding these food groups in the context of Paleolithic nutrition.
Criticisms?
Another small study that didn’t exactly follow what is traditionally thought of as a Paleo diet.
Our take
The results of the study are impressive, however, larger scale studies are needed to give more insight, and this study cannot stand for the proposition that saturated fat is healthy for all individuals.
Overall summary
- Short term studies suggest that a lower fat Paleo diet may be beneficial for a variety of metabolic disorders, is better than “average” diets and is no worse than traditional healthy diets in the short term.
- Long term issues surround the impact of a Paleo diet on health, especially the more extreme forms with very low carbohydrate intake.
- The role of saturated fat in the Paleo diet remains unclear, and the studies do not support the idea that saturated fat is beneficial. At best they are neutral.
- Despite the fact that it applies to some individuals genetically, the “saturated fat is harmless” message advanced by the Paleo community is being oversold to the public. Some of the most prominent Paleo diet studies actually reduced saturated fat intake in their subjects.



