Do B Vitamin Supplements Increase Cancer Risk?
Genes Mentioned

Contents
The common thinking in supplement circles that because B vitamins are water soluble, they can be taken in larger and larger doses with no consequences. This isn’t the whole story. In fact, at certain populations and at certain doses, supplementing with B vitamins seems to increase the risk for certain types of cancers.
I’ve summarized the findings in a giant table to the end of the post, but I’ll go through some studies to describe the headline findings, and importantly the doses of B vitamins and groups assessed.

Unlock Your Personalized Nutrition & Supplement Report
Gene Food uses a proprietary algorithm to divide people into one of twenty diet types based on genetics. We score for cholesterol and sterol hyperabsorption, MTHFR status, histamine clearance, carbohydrate tolerance, and more. Where do you fit?
JAMA Study
The authors of this JAMA study prospectively set out to assess cancer risk in relation to vitamin B dosing.
In this study, 6,837 patients from two Norwegian patient groups, with existing heart disease, were treated with certain B vitamins or a placebo between 1998 and 2005. Interestingly, the study authors identify a significant increase in cancer risk when patients supplemented with folic acid (0.8 mg/d) and vitamin B12 (0.4 mg/d) for 39 months.
In both instances lung cancer risk was especially increased.
This is quite a striking effect considering the doses and how closely these could mimic many people’s daily supplement regimens. Doses of 0.8mg of folic acid and 0.4mg of B12 are very common in dietary supplements, so this study offers a real warning sign to those who mega dose B vitamin supplements over a long period of time.
When you see lung cancer the immediate thought is smoking, so it’s no surprise that based on the above study two quite similar papers came out in 2012 and 2013.
The obvious question is what do B vitamins do to those who are already at risk of cancer? Does supplementing with B vitamins “turn on” the cancer?
Long-Term B Vitamin Use and Lung Cancer Risk
Enter this 2017 study which looked at 77,118 men and women between the ages of 50 and 76 with defined vitamin B intakes over 10 years, these defined intakes were taken as either multivitamins or individual dosings and a huge raft other metrics were also recorded.
Their take home findings were pretty startling:
- In women, high dose vitamin B6, B12 or folic acid was not associated with an increased cancer risk.
- In men both vitamin B6 (20 mg/d – HR 1.82) and vitamin B12 (0.55 mg/d – HR 1.98) were associated with an increased lung cancer risk.
- For current smokers this risk was even worse (B6 HR 2.93 and B12 HR 3.71).
- This was only observed for single supplements not multivitamins.
Quite a lot to digest there, but there are some interesting things we can draw out from these findings. Firstly, the doses used are higher than in the retrospective studies, and the lower doses used in these studies did not report any significant association.
So only the highest doses of B6 and B12 had any association. Secondly, smoking while on these high doses seems to be a big risk, the combined HR from B6 and B12 should be concerning for smokers.

Gentle Support Methylated B Complex
Tired of huge B vitamin doses? Gentle Methyl is made for people who prefer a measured dose of methylated B vitamins over the megadose formulas that dominate the market.
Is vitamin B2 protective?
Finally, the lack of effect from multivitamins is very interesting. One possible hypothesis is that the presence of vitamin B2, which other studies showed was protective, can block the increased cancer risk of B6 and B12 at high doses. Unfortunately, this study didn’t assess vitamin B2 alone so we can’t say for sure but the hypothesis fits with the data available so far.
Evaluating B Vitamin Supplements
The obvious concern here is dose.
We want doses of folic acid of less than 0.8mg, and B12 at less than 0.4mg.
It’s also preferable to have B6 at low doses, both because of the cancer issue, as well as because of some data that indicates B6 can cause nerve damage at higher doses. For example, when I have experimented with 50mg doses of B6 as a way to stimulate diamine oxidase production to clear excess histamine, I have experienced tingling in mu feet, which is definitely no bueno.
We’ve also theorized that pairing these B vitamins with B2, or other antioxidants, could have a protective effect, so the data seems to indicate that supplementing with B vitamins is safer as part of a multivitamin. Ok, so armed with that knowledge, let’s explore some of the options out there for supplementing with B vitamins and see if we can identify some good products.
Vitamin B12 dosing
To begin, Vitamin B12 seems to be the most popular B vitamin to supplement with, and the market has responded with mega dose supplements everywhere. These supplements usually list doses in terms of micrograms. You’ll most commonly see 1,000 and 5,000 mcg doses. This converts to 1 mg and 5 mg respectively.
Tying this back into the JAMA study, we see that a 1 mg dose is more than double the 0.4 mg dose of B12 that was associated with an increased risk of cancer in the Norwegian population. 1 mg of B12 represents 16,667% of your daily B12 intake. So, in the world of B12 supplements, we want a product that offers methylcobalamin (the quality form of B12) and a dose of 500 mcg or less.
Take home message
The take home message from all these studies is quite clear. High doses of B6 and B12 have a strong cancer promoting effect, especially in men, with male smokers being at the highest risk. This risk isn’t seen with lower doses, or in multivitamins (potentially because of the protective B2 effect).
So check your supplement doses!
While these vitamins are key in the one carbon cycle, and may be helping with certain SNPs it is very possible that you could get away with a much lower dose. For those thinking of starting B vitamin supplements to help with their SNPs we would always recommend starting at lower doses (1/3 of a capsule or lower) and keeping a diary to record what effect these have, rather than jumping in with the maximum dose.
More is not always, or even usually, better when it comes to supplements.
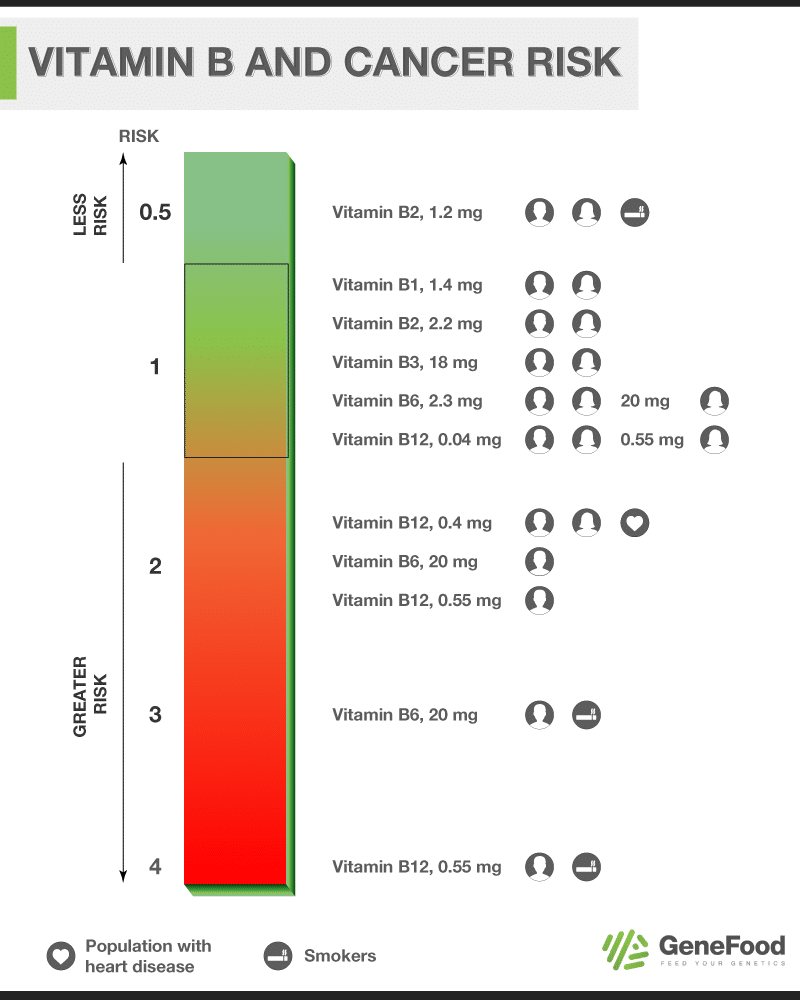
B Vitamin and Cancer Risk Diagram
We put together this visual to chart the various studies that have evaluated B vitamin supplements and cancer risk.

Gentle Support Methylated B Complex
Tired of huge B vitamin doses? Gentle Methyl is made for people who prefer a measured dose of methylated B vitamins over the megadose formulas that dominate the market.



The chart shows Vit B12 1.5 mg having lower risk than 0.04 mg or 0.55mg ! Was that a typo?
I’ve seen several posts mentioning cycling supplements, do you have a post specifically on that? I searched and couldn’t find one, so if there isn’t one I hope you write it!
I am also interested in learning bout cycling supplements.
Hi,
Could you add the reference for that 2017 study?
Also, based on the JAMA study, I’m not convinced b12 is a problem since there was no group that supplemented with just b12 so no way to know if b12 has anything to do with the effect or if it’s just the folic acid. The researchers themselves say the effect is probably mediated by the folic acid in the article discussion. Additionnally, they used cyanocobalamin which you say yourself is the “lower quality” form of b12. Thridly, the baseline level of b12 was 477 pg/mL and was raised to 761 pg/mL in the study group. My level is 210 pg/mL and my doctor says it’s fine, it’s “in the range”. But I feel better when I supplement with 2400 mcg (methylcobalamin + adenosylcobalamin) so I’m inclined to continue. Of course I want to take cancer risk seriously but based on my non-expert analysis of this study, I’m tempted to continue supplementing. Thoughts?
Appreciated your thoughts and review!